Reduce "Off" Time: Practical Ways to Cut Parkinson's Wearing‑Off
Wearing‑off — those moments when your meds stop working and symptoms return — can be the hardest part of living with Parkinson's. You don't have to accept long, unpredictable off periods. Small changes often bring real, daily improvements.
Quick fixes you can try now
Start by tracking when off episodes happen. Keep a simple diary for a week: note the time your dose was taken and when symptoms returned. Patterns show up fast and give your doctor real clues.
Timing matters. Many people find splitting doses into smaller, more frequent amounts smooths control. Set alarms or use a pill box so doses are consistent. Also watch protein: high‑protein meals can block levodopa absorption. Try taking medication 30–60 minutes before meals or move protein to later in the day.
Carry a rescue option. Short-acting rescue meds — like apomorphine (under doctor guidance) or quick‑acting levodopa formulations — can break a bad off spell. Ask your neurologist about safe rescue plans and how to use them.
Longer‑term strategies that often help
If quick fixes don’t cut it, there are well‑tested medical options. Adding a COMT inhibitor (entacapone), an MAO‑B inhibitor (rasagiline or safinamide), or a dopamine agonist can extend levodopa’s effect and reduce off time. Newer extended‑release levodopa (Rytary) or patches like rotigotine offer steadier levels through the day.
For severe, fluctuating off time, continuous therapies work well. Duopa (intestinal levodopa infusion) and subcutaneous apomorphine pumps give steady medication and can shrink off periods dramatically. Deep brain stimulation (DBS) is another option for people who qualify — it reduces fluctuations for many patients.
Don’t forget non‑drug tools. Regular exercise, targeted physical therapy, and speech work can make off periods less disabling. Practice simple movement routines you can use when symptoms start: weight shifts, big steps, or rhythmic cues often help mobility quickly.
Watch side effects. Adding drugs often brings nausea, sleepiness, or impulse changes. Track new symptoms and report them. Never stop or change doses suddenly — that can make things worse.
Finally, partner with a specialist. A movement‑disorder neurologist will tailor the mix of timing, add‑on meds, rescue options, or device therapies. Bring your diary to appointments — it saves time and leads to smarter changes.
Off time is frustrating, but practical steps — better timing, rescue plans, add‑on meds, continuous delivery, and rehab — cut it down for many people. Talk to your care team and try one change at a time so you know what helps you most.
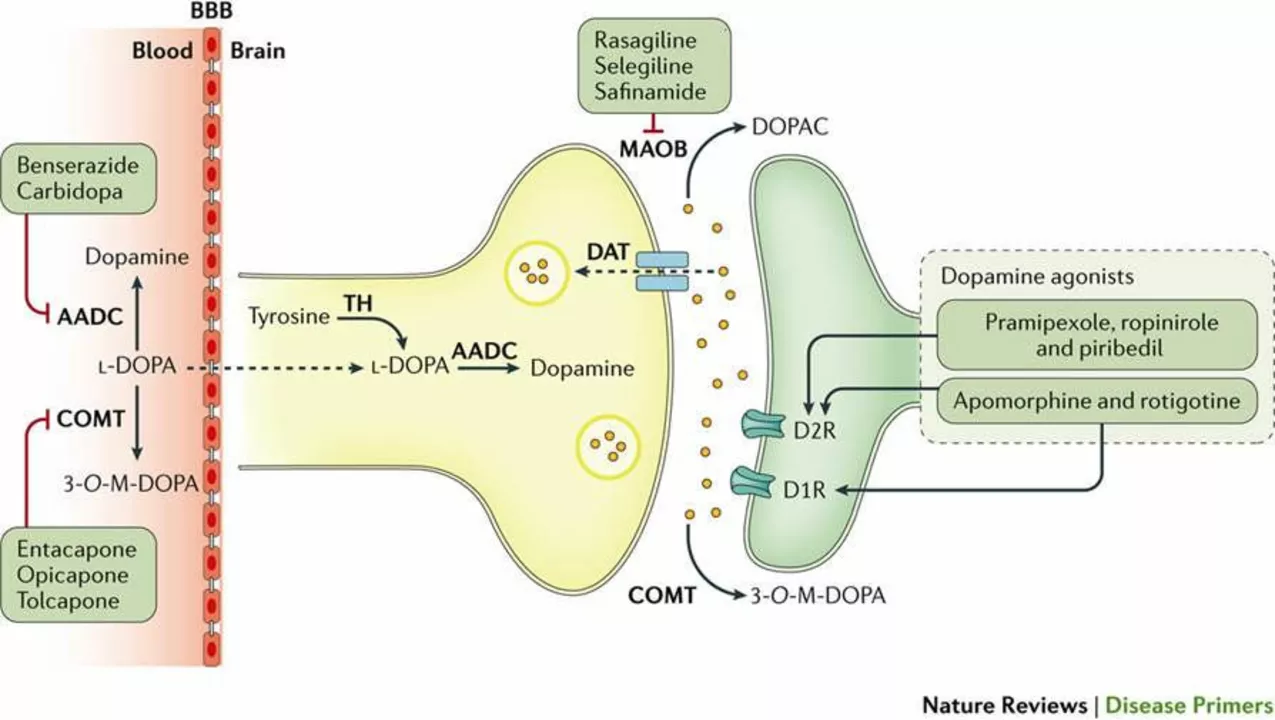
How carbidopa-levodopa-entacapone can help reduce "off" time in Parkinson's patients
Apr 27, 2023, Posted by Mike Clayton
As a Parkinson's patient, I've found that carbidopa-levodopa-entacapone can significantly help in reducing "off" time. This combination medication works by increasing dopamine levels in the brain, which is crucial for controlling movement and coordination. By enhancing the effectiveness of levodopa, entacapone allows for a smoother and more stable response to the treatment. Consequently, this reduces the frequency and duration of "off" periods, during which symptoms can worsen. Overall, carbidopa-levodopa-entacapone has made a significant difference in managing my Parkinson's symptoms and improving my quality of life.
MORESEARCH HERE
Categories
TAGS
- treatment
- online pharmacy
- dietary supplement
- side effects
- medication safety
- generic drugs
- medication adherence
- health
- dietary supplements
- health benefits
- online pharmacy Australia
- generic substitution
- adverse drug reactions
- thyroid disorders
- gabapentin
- treatment option
- calcipotriol
- blood pressure
- erectile dysfunction
- closer look
