Betamethasone: Uses, Safety, and Practical Tips
Betamethasone is a strong corticosteroid used to reduce inflammation. You’ll find it as creams, ointments, lotions, injections, and sometimes eye or ear drops. Doctors prescribe it for eczema, psoriasis, allergic rashes, severe dermatitis, and certain autoimmune conditions. It works fast to calm redness, swelling, and itching, but it’s powerful, so using it right matters.
Topical use is common. Apply a thin layer to clean, dry skin once or twice daily as directed. Don’t use on infected skin unless your doctor adds an antibiotic. Avoid long courses on the face, groin, or armpits because the skin there is thin and absorbs more steroid. If you need treatment longer than a few weeks, the prescriber should review progress and consider stepping down strength or switching to alternatives.
Injections or systemic betamethasone treat severe inflammation when topical treatment won’t cut it. These routes carry more risk of side effects like high blood sugar, mood changes, sleep issues, and weakened bones if used long term. If you have diabetes, high blood pressure, or a history of osteoporosis, tell your doctor before starting systemic steroids. They may need to monitor you more closely.
Common local side effects from creams include skin thinning, stretch marks, lightening of skin color, and easy bruising. If irritation, worsening rash, or signs of infection happen, stop use and call your prescriber. For injectable or oral forms, watch for weight gain, facial swelling, increased appetite, or mood swings. If you notice sudden vision changes, severe abdominal pain, or signs of infection like fever, get medical help fast.
How to use betamethasone safely
Follow the exact dose and schedule your provider gives. Don’t increase frequency to speed results. Use only on the areas mentioned, and wear gloves if applying to someone else. Wash hands after applying unless treating the hands. Avoid occlusive dressings unless directed; they increase absorption and risk of side effects. Keep treatments out of reach of children.
Practical tips and interactions
Combine betamethasone with moisturizers for better control of dry skin, applying the moisturizer first unless told otherwise. Avoid mixing with other topical products without advice. Some medicines and vaccines behave differently if you’re on systemic steroids, so inform any healthcare professional you see. Pregnant or breastfeeding? Discuss risks and benefits with your doctor—topical use is often safer than systemic, but guidance matters.
Short courses of betamethasone can bring quick relief, but think long term about controlling triggers, skin care routines, and steroid-sparing options. When in doubt, ask your pharmacist or prescriber for simple, practical advice tailored to your situation.
Store all steroid products at room temperature away from heat and light, and keep liquids tightly closed. Dispose of unused injections and expired creams properly through a pharmacy takeback or local hazardous waste program. If you travel, pack prescribed amounts and carry a copy of your prescription. Report any unusual side effect to your healthcare team so problems get fixed early. Knowing when to stop or taper prevents rebound flares. Always ask questions.
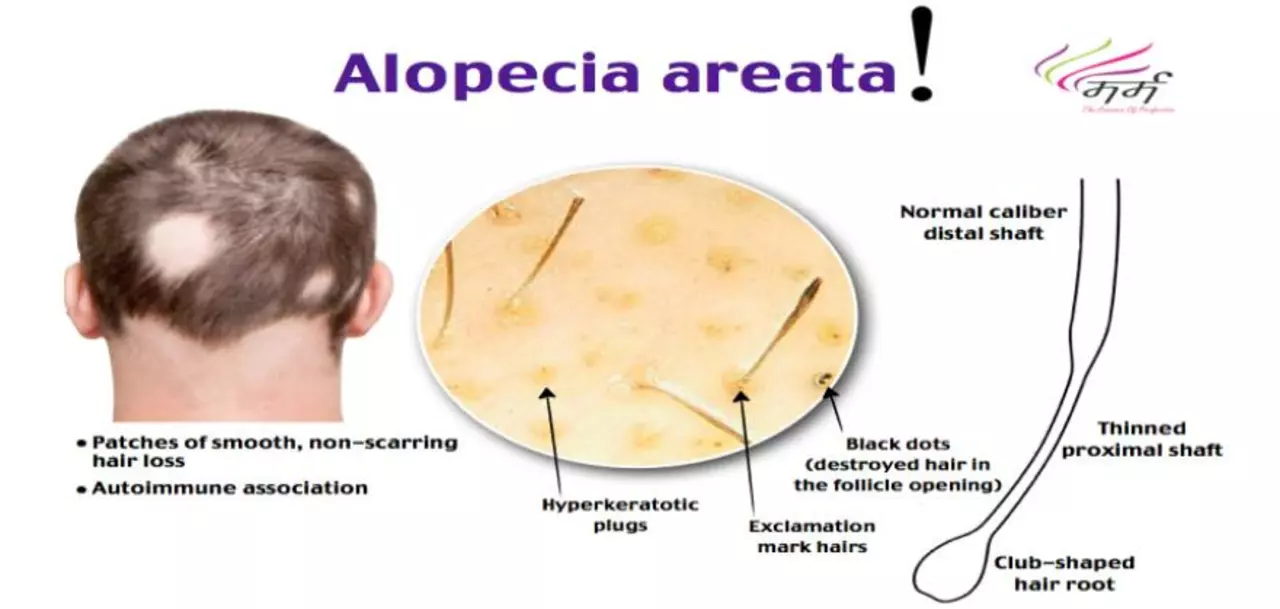
The use of betamethasone in the treatment of alopecia areata
May 19, 2023, Posted by Mike Clayton
As a blogger, I've recently come across some fascinating information on the use of betamethasone in treating alopecia areata. It turns out that this potent corticosteroid can be quite effective in managing this hair loss condition. The treatment usually involves injections into the scalp which helps reduce inflammation and stimulate hair growth. While it may not work for everyone, many patients have reported significant improvement with this treatment option. It's important to consult with a healthcare professional before considering betamethasone, as there are potential side effects to be aware of.
MORESEARCH HERE
Categories
TAGS
- treatment
- online pharmacy
- dietary supplement
- side effects
- medication safety
- generic drugs
- medication adherence
- health
- dietary supplements
- health benefits
- online pharmacy Australia
- generic substitution
- adverse drug reactions
- thyroid disorders
- gabapentin
- treatment option
- calcipotriol
- blood pressure
- erectile dysfunction
- closer look
